Shoulder Joint Arthritis: A Summary
Glenohumeral arthritis is a degenerative condition affecting the shoulder. The glenohumeral joint is the main shoulder joint where the ball meets the shoulder socket. This condition leads to the deterioration of the articular cartilage, causing pain, stiffness, and reduced function of the shoulder.
Common Symptoms of Shoulder Arthritis
Pain: The primary symptom is pain, often felt deep within the shoulder. The pain can be exacerbated by activity and may become more constant as the condition progresses. Pain at night, particularly when lying on the affected shoulder, is common.
Stiffness: Patients frequently experience a reduction in the range of motion, making it difficult to perform everyday activities, such as reaching overhead or behind the back.
Crepitus: A grinding or clicking sensation (crepitus) may be felt during shoulder movement due to the rough surfaces of the bones rubbing together.
Weakness: Muscle weakness, particularly in the rotator cuff and deltoid muscles, can occur as a result of disuse or as the condition progresses.
Swelling and Tenderness: Although less common, some patients may experience swelling and tenderness around the joint.
Causes of Shoulder Arthritis:
Osteoarthritis (Primary Glenohumeral Osteoarthritis): The most common cause of glenohumeral arthritis is osteoarthritis, a wear-and-tear condition where the cartilage gradually breaks down over time, leading to bone-on-bone contact.
Rheumatoid Arthritis: An autoimmune disorder where the body’s immune system attacks the synovium (the lining of the joint), leading to inflammation, pain, and cartilage destruction.
Post-Traumatic Arthritis: This form occurs following a shoulder injury, such as a fracture, dislocation, or severe rotator cuff tear, which can accelerate cartilage degeneration.
Rotator Cuff Tear Arthropathy: A condition where a chronic rotator cuff tear leads to changes in shoulder mechanics, resulting in arthritis and joint degeneration.
Avascular Necrosis: A condition where the blood supply to the humeral head is disrupted, causing the bone to die and collapse, leading to secondary arthritis.
Inflammatory Arthritis: Conditions like lupus or psoriatic arthritis can also cause inflammation of the shoulder joint, leading to arthritis.
Biology of Shoulder Arthritis:
Cartilage Degradation: The hallmark of glenohumeral arthritis is the breakdown of hyaline cartilage, which normally cushions the joint and allows for smooth movement. As the cartilage wears away, the underlying bone becomes exposed and can rub against the opposing bone, leading to pain and joint damage.
Inflammation: Inflammatory forms of arthritis (e.g., rheumatoid arthritis) involve the immune system attacking the joint, leading to chronic inflammation. This inflammation not only damages cartilage but can also erode the bone, further worsening the condition.
Synovial Fluid Changes: The synovial fluid, which lubricates the joint, can become less effective in arthritis due to changes in its composition or an inflammatory environment, leading to increased friction and joint damage.
Current Treatments for Shoulder Arthritis:
Non-Surgical Treatments:
Physical Therapy: Exercises and stretches to improve the range of motion, strengthen the shoulder muscles, and reduce stiffness.
Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen, Motrin, naproxen, Aleve, Tylenol arthritis, etc. are commonly used to reduce pain and inflammation. In some cases, corticosteroids (e.g., prednisone) may be prescribed for short-term relief.
Activity Modification: Patients may be advised to avoid activities that exacerbate symptoms, such as heavy lifting or repetitive overhead movements.
Injections: Corticosteroid injections can provide temporary relief from pain and inflammation. Hyaluronic acid injections, which aim to lubricate the joint, are also sometimes used.
Heat and Cold Therapy: Application of heat can help relieve stiffness, while cold packs can reduce inflammation and pain.
Surgical Treatments:
Arthroscopy: A minimally invasive procedure where small instruments are inserted into the joint to clean out debris, smooth rough cartilage, or remove loose bodies. It is usually more effective in the earlier stages of arthritis. However, it generally only provides partial pain relief for a short period of time. For that reason, it is rarely used.
Hemiarthroplasty: Involves replacing only the humeral head with a prosthesis, leaving the natural glenoid intact. It is used in cases where the glenoid cartilage is relatively preserved.
Anatomic Total Shoulder Replacement (TSA): Both the humeral head and the shoulder socket are replaced with prosthetic components. This is the standard treatment for advanced glenohumeral arthritis.
Reverse Total Shoulder Replacement (RSA): Used primarily in cases of arthritis combined with severe rotator cuff tears. This procedure reverses the normal anatomy of the shoulder joint to allow the deltoid muscle to compensate for the deficient rotator cuff.
Future Treatment Options Being Investigated:
Biologic Therapies:
Stem Cell Therapy: Research is ongoing into the use of stem cells to regenerate damaged cartilage in the shoulder joint. These therapies aim to promote the body’s natural healing processes to restore joint function and reduce pain. This is currently considered experimental, lacks scientific evidence and the risks are not well understood. For that reason, Stem Cell Therapy is generally not recommended.
Platelet-Rich Plasma (PRP): PRP involves injecting a concentration of a patient’s own platelets into the shoulder joint. The growth factors in PRP may help reduce inflammation and promote tissue healing. PRP is considered safe and currently used in some cases. However, its efficacy is still under investigation. Corticosteroid (steroid) injections are often considered equally or more effective.
Advances in Prosthetic Design:
Customized Implants: The development of 3D-printed and patient-specific implants allows for better-fitting prostheses tailored to an individual’s unique anatomy. These advances may lead to improved outcomes and longer-lasting joint replacements. Dr. Harold will commonly use custom 3D-printed implants when they are needed for complex shoulder reconstruction cases.
Smart Implants: Future shoulder implants may incorporate sensors or other technology to monitor joint health, detect early signs of wear, and provide feedback to patients and surgeons to optimize recovery and longevity.
Cartilage Regeneration Techniques:
Tissue Engineering: Scientists are working on ways to grow new cartilage in the lab using a combination of cells, scaffolds, and growth factors. This engineered cartilage could one day be used to replace damaged tissue in the shoulder joint.
Mosaicplasty and Autologous Chondrocyte Implantation (ACI): These techniques, which are more commonly used in knee arthritis, involve transplanting healthy cartilage from one part of the joint to the damaged area. Researchers are exploring the potential of adapting these techniques for the shoulder.
Summary of Shoulder Arthritis:
Glenohumeral (shoulder ball and socket) arthritis is a debilitating condition that significantly impacts quality of life. Current treatments focus on pain management, maintaining function, and in advanced cases, shoulder joint replacement. Dr. Harold specializes in shoulder joint replacement/reconstruction, including anatomic total shoulder replacement, reverse total shoulder replacement, and revision (re-do) shoulder replacement.
Future therapies are not currently well established yet, but hold the promise of more effectively restoring joint health and function. Advances in biologic therapies and prosthetic design, as well as ongoing research into cartilage regeneration, may revolutionize the way glenohumeral arthritis is treated in the coming decades.
Normal
Arthritis
Normal
Cuff Tear Arthropathy
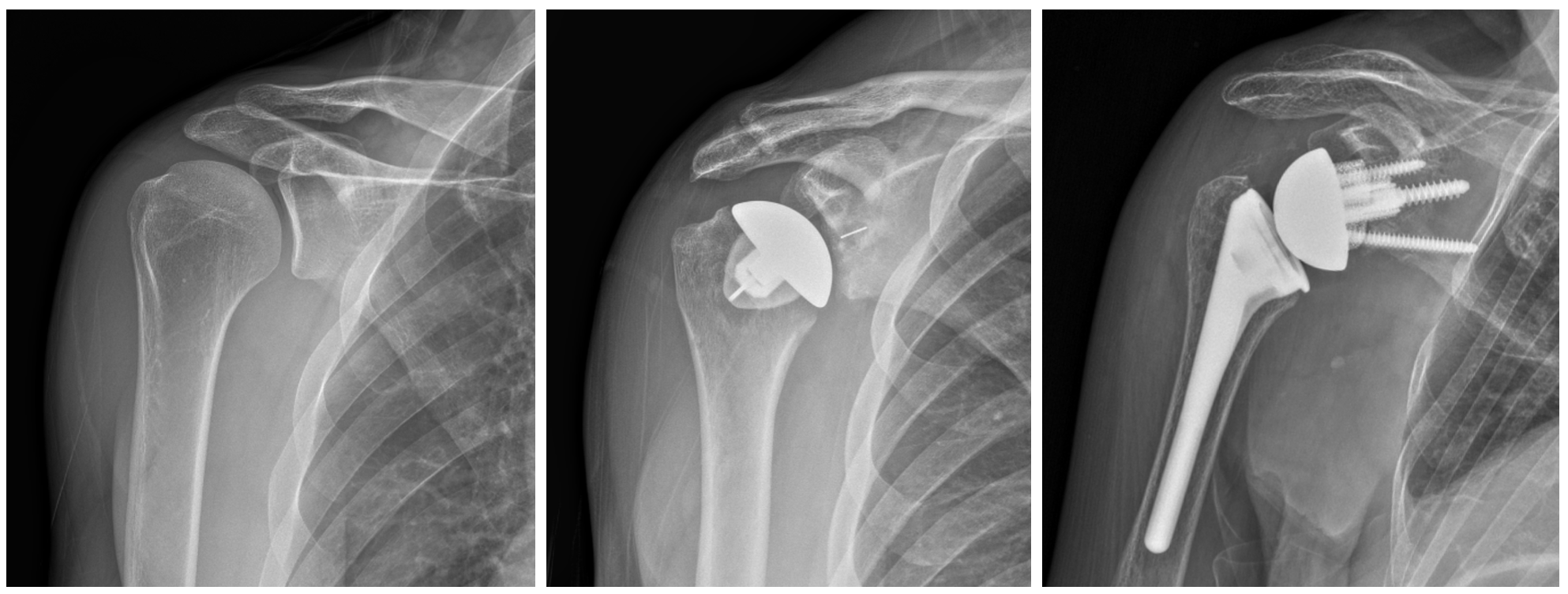
Anatomic
Reverse
Shoulder:
Shoulder Fractures
Revision (re-do) Shoulder Replacement
Elbow:
Elbow Fractures
Cubital Tunnel Syndrome
Elbow Arthritis
Radial Head Fractures
Hand/Wrist:
Cubital Tunnel Syndrome
Hand Fractures
Scaphoid Fractures
Tendon Lacerations